Brief

At a Glance
- Bain survey data shows that physician satisfaction at health systems consistently lags that of physician-owned practices.
- Health systems have many professional dimensions with low satisfaction and high potential for improvement, such as leadership alignment and physician autonomy.
- To raise satisfaction and build a culture of trust, health-system-led practices can apply four lessons from physician-led ones.
There’s a widening chasm in the healthcare workforce: Physicians at practices owned by or serving hospitals and healthcare systems are almost three times more likely to be dissatisfied than those at practices owned by physicians.
Since 2017, the Net Promoter Score℠—a measure of employees’ likelihood to recommend their employer—at US health-system-led organizations has been 25 to 40 points lower than at physician-led ones, according to Bain’s Frontline of Healthcare Survey (see Figure 1).
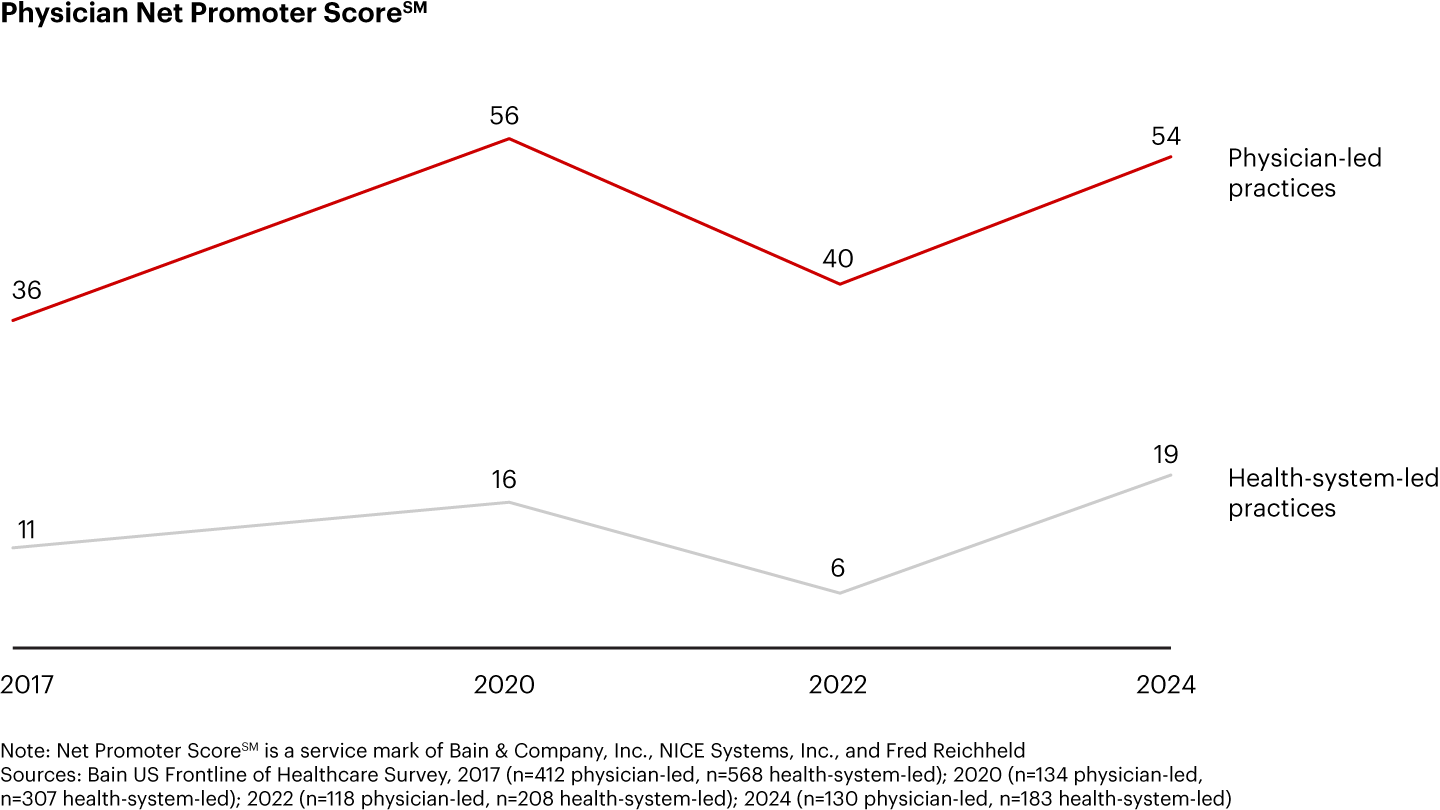

This shift in the ownership model has been one of the greatest changes in the US healthcare system over the past 30 years. In the 1990s, around 70% of physicians worked in independent practices that were owned by physicians themselves. Most of these practices were small, employing fewer than five doctors, and resembled a family business. They aligned the interests of managers and physicians because they were often one and the same.
Fast-forward to today, and only around 47% of physicians work in physician-led practices, while approximately 41% work in health-system-led ones, according to 2022 American Hospital Association (AMA) data.
As healthcare has moved toward a system-led approach, many practices seem to have lost the secret sauce of the original physician practice model. Now, they are at high risk of losing unhappy physicians. Across healthcare organizations, physicians who are detractors of their employers are six times more likely to switch employers than satisfied promoters. Nearly one-quarter of physicians in health-system-led organizations are considering switching employers, compared to just 14% in physician-led ones. Among those seeking to leave, 37% want to move to physician-led practices.
It's a tough time to lose employees. The US clinician shortage is intensifying competition for talent. And a short-staffed system with disgruntled employees is hardly a selling point for patients. It’s a lose-lose situation—bad for patients and bad for bottom lines.
The stakes have never been higher for health-system-led organizations to improve the physician experience. Learning from the success of physician-led organizations may be the best way to get there.
What physician-led practices get right
Our recent Frontline of Healthcare Survey shows that not all professional dimensions are equal in the eyes of physicians. Some have a disproportionately high potential to delight or disappoint—areas we call “star dimensions.” For physicians at health-system-led organizations, the most critical star dimensions are compensation, staffing and workload, and autonomy (see Figure 2a). When organizations neglect these factors, they often create dissatisfied detractors who are significantly more likely to switch employers. But when practices focus on these dimensions, they generate loyal, enthusiastic promoters who are more likely to stay and recommend their employer to others.
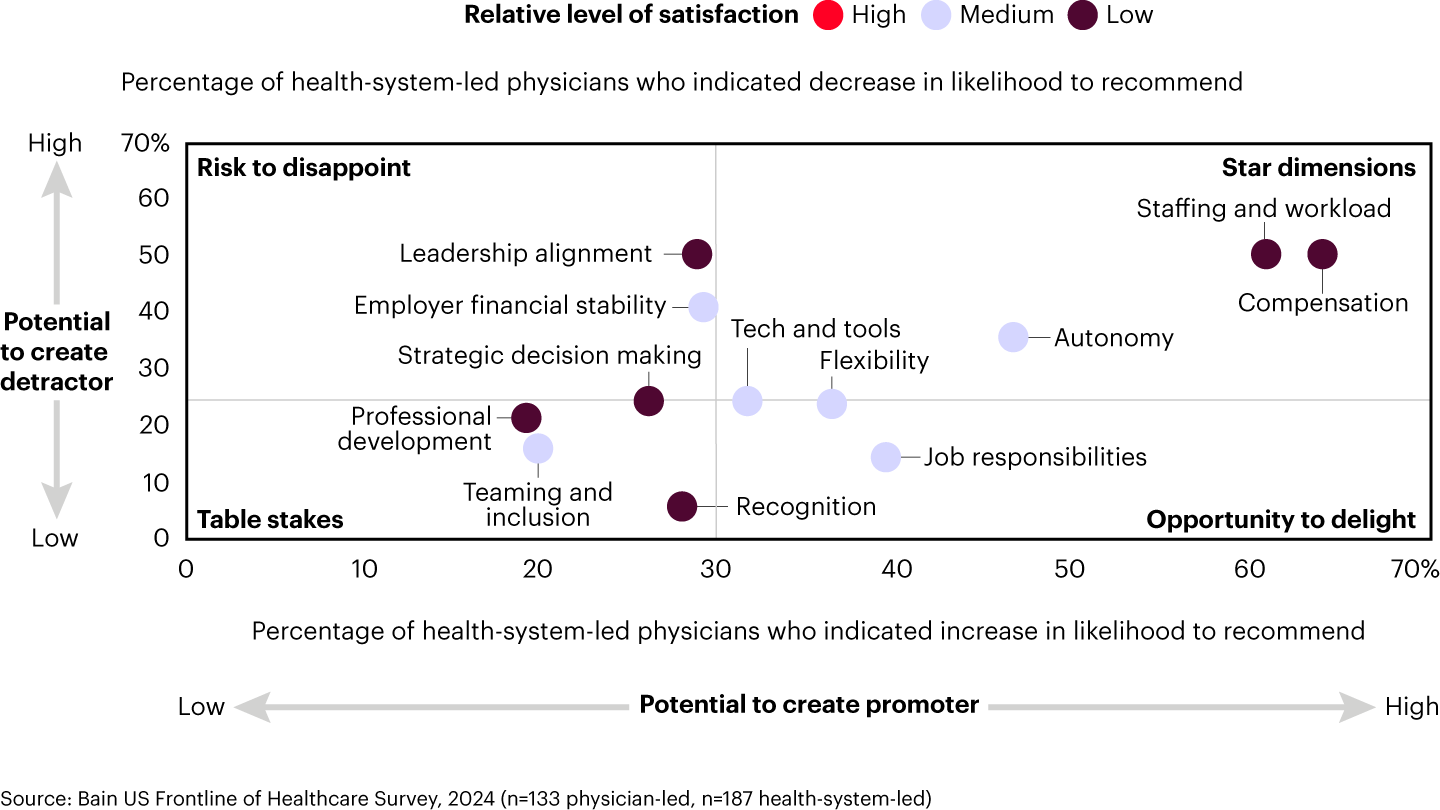


The top priorities to improve the physician experience in health systems are clear: fair compensation, adequate staffing and manageable workloads, leadership alignment, involvement in strategic decision making, and autonomy. Currently, these dimensions have low to medium satisfaction, but improving them can significantly boost Net Promoter Scores.
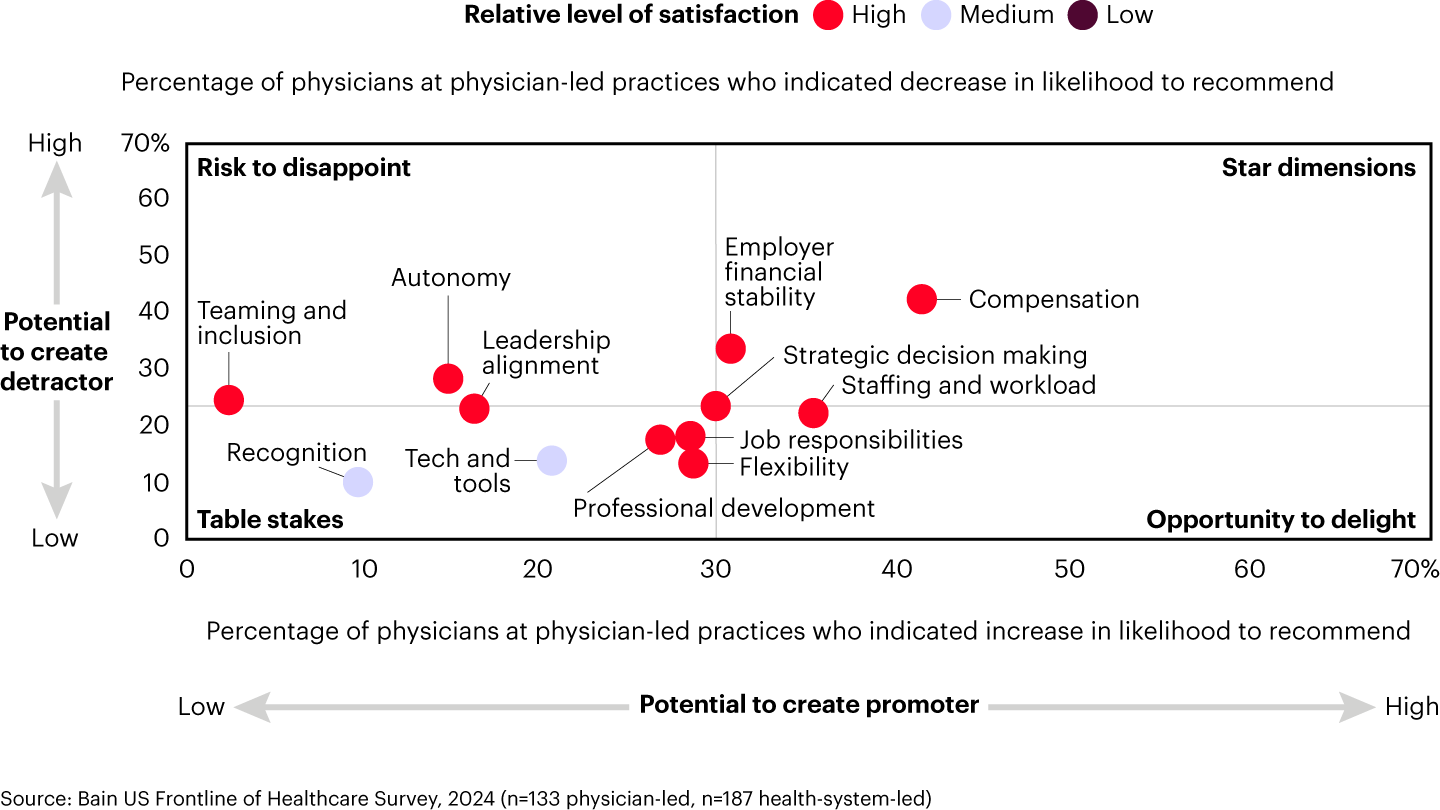
Physician-led organizations score considerably higher in satisfaction across all professional dimensions (see Figure 2b). Their average satisfaction ranges from roughly 70% to 90%, compared to 50% to 75% in health-system-led practices.
The gap in satisfaction mirrors other disparities we see in the physician experience. For example, 87% of physicians in physician-led practices say they have access to the supplies and equipment they need, vs. only 68% in health-system-led ones. Similarly, 78% of physicians in physician-led practices report that their organizations have effective processes and workflows, vs. 59% in health-system-led ones. Furthermore, a higher proportion of physicians at physician-led organizations report having employee-experience mechanisms, such as a system to address employee feedback and a culture of recognition. These physicians also have a greater sense of belonging and feel less worn out.
Even when employer performance on a specific dimension declines, overall satisfaction at physician-led practices is unlikely to drop as sharply as it does in health-system-led settings. We attribute this resilience to one differentiating factor: a culture of trust.
Several studies have examined the characteristics of trusted physician-leadership relationships, including managers’ care for employees’ well-being, ethics, availability, and competence. But one factor is most associated with trust in management: an empowering work environment. We believe it helps buffer overall satisfaction in physician-led settings, even if the quality of one professional dimension declines.
Borrowing best practices from physician-led practices
Bridging the gap in physician satisfaction will require targeted changes within healthcare systems. There is no single cause for dissatisfaction, meaning individual organizations need to identify and address the root causes among each group of physicians. But building trust through an empowering work environment can be a guiding principle for all organizations.
Four pragmatic changes can help health-system-led organizations replicate the best practices of physician-led organizations, boosting satisfaction and doing right by their employees.
1. Establish a clear physician value proposition.
Health systems can start by defining a compelling physician value proposition that differentiates them from other organizations. Which qualities do they want to be known for? What unique benefits and experiences make their organization attractive to physicians?
The best value propositions aren’t crafted in a silo by the leadership team but instead by a cross-functional group that includes physicians across the system. This inclusive approach fosters greater leadership alignment, which is key to employee satisfaction. In fact, we’ve found a lack of leadership alignment has the highest likelihood of disappointing health-system-led physicians. And only about 60% of these physicians say they are happy with their organization’s leadership alignment. Alignment not only reinforces the shared goals but also harmonizes the leadership team’s efforts, ensuring cohesive decision making and action.
A strong value proposition is ambitious and aspirational, yet tangible and attainable. By aligning leaders and engaging physicians across the organization, it creates a unified direction. Everyone feels energized and empowered to work toward the shared vision.
2. Involve physicians in decision making.
One of the most effective ways to empower physicians and build trust is to involve them in strategic decisions, particularly those that affect their work. In 2024, physicians engaged in strategic decision making at health-system-led organizations reported an overall Net Promoter Score of 48, compared to –31 from their unengaged counterparts. Those results are consistent with what we’ve seen over the past decade.
Not surprisingly, 81% of physicians in physician-led organizations say they are satisfied with their involvement in strategic decision making, compared to only 50% in health-system-led organizations.
To involve physicians more, organizations first need a clear view of the “what, who, how, and when” of decision making. Tools like Bain’s RAPID® (Recommend, Agree, Perform, Input, and Decide) model can help organizations clarify decision-making roles across multiple stakeholders, by defining who recommends a course of action, who must agree, who provides input, and who ultimately decides.
Organizations can tap into the unique perspectives of their people by identifying the right areas for physician involvement, such as clinical protocols, technology adoption, and patient-care initiatives. This will enhance decision quality and foster a sense of ownership and engagement, bolstering trust between physicians and leadership.
3. Enhance digital tools and technology.
Technology and tools are one dimension where health-system-led organizations can delight physicians. Yet compared to their physician-led counterparts, these organizations often struggle to optimize technology. Aspects of acquisitions and expansions, such as data interoperability and systems integration, are often overlooked, leading to inefficiency. And despite greater access to capital, these practices’ larger size complicates digital investment decisions. Health-system-led practices typically cater to a broader group rather than specific subsets of physicians and their diverse clinical and operational needs.
But the most significant challenge is cutting through the noise and hype to prioritize the digital and tech investments that will tangibly improve the physician experience and patient outcomes. Leading organizations develop a clear digital strategy to guide their choices and a well-defined execution plan to deploy and scale prioritized initiatives.
Take generative AI, for instance. It’s a massive opportunity for health systems to reduce administrative burdens and enhance clinical decision-making support. However, 75% of administrators say their organization lacks a set list of use cases. More than 70% say they don’t have a clear vision, timeline, roadmap, or the critical talent and capabilities needed to implement and utilize generative AI.
By analyzing the root causes of their shortcomings and addressing the gaps, health systems will be better positioned to embrace digital transformation. This, in turn, will equip physicians with the necessary infrastructure to deliver more effective, high-quality care.
4. Implement a closed-loop feedback system.
Most hospital administrators and clinicians say they struggle to recruit and retain physicians, especially in health-system-led organizations. And sending out annual staff surveys with high-level questions or failing to follow up on feedback isn’t going to move the needle on the employee experience.
It’s imperative that health systems understand what matters most to their physicians, as well as their unmet needs and pain points. Top employers assess which changes will have the greatest effect so that they can make the right investments and trade-offs, focusing on areas with the highest risk of disappointment and the lowest satisfaction.
The sheer size of most health-system-led organizations makes informal methods of tracking sentiment, like corridor chats, unfeasible. Scale underscores the need for an effective system, like the Net Promoter System®, to assess and act on feedback at an organization-wide level.
In closed-loop systems, leaders regularly collect detailed feedback and systematically analyze it for recurring themes, root causes, and opportunities for improvement. They route those opportunities to the appropriate teams who can determine next steps and track implementation. The loop is closed when leaders communicate the changes back to physicians. This comprehensive approach not only propels continual improvement but also shows physicians that leaders value their opinions.
In replicating the best practices of physician-led practices, health systems will likely reap the benefits of a more satisfied, engaged, and loyal workforce, such as higher retention rates, lower turnover costs, and better patient outcomes. It will be a challenging transition, but these steps can set health systems on the right path toward building an enduring culture of trust—the heartbeat of a thriving organization.