Brief

At a Glance
- New primary care models from nontraditional players—such as advanced primary care providers, retailers, and payers—aim to deliver more efficient care, improve patient outcomes, and lower costs.
- By 2030, these innovative reimbursement, care, and ownership models could capture as much as a third of the US primary care market.
- Payers, health systems, and investors will need to make strategic choices to determine where to play and how to win over the next decade.
For a decade now, primary care has seen a steady stream of new business and clinical models, including those from advanced primary care (APC) providers, retailers, and payers. By 2030, the space won’t look the same at all: Bain expects these nontraditional primary care providers to make up as much as a third of a market that, today, is still dominated by traditional providers in fee-for-service arrangements.
Consider, for example, the entry of APC disrupters like Oak Street Health, new retailer partnerships like the one between Walgreens Boots Alliance and VillageMD, and the launch of UnitedHealth Group’s OptumCare.
These are harbingers of more to come: creative, innovative models that deliver more efficient care, improve patient outcomes, and lower total costs. Over the course of the next decade, rising costs, consumerism, labor shortages, demographic shifts, and digital disruption will continue to alter the primary care landscape. Together, these forces are already reshaping the foundations of primary care—including reimbursement, care, and ownership models—ushering in a new era of industry-transforming innovation and competitive dynamics.
Reimbursement models in 2030
The shift from fee-for-service to fee-for-value reimbursement models has been one of the most significant sources of innovation in primary care, a trend we expect will only accelerate.
Both independent and payer-owned APCs will continue playing a major role here. Although APC disrupters make up just a fraction of the total market, they are following the profit pools and spearheading population-specific models that aim to operate in full capitation. What’s more, they are already demonstrating better clinical outcomes, lower total cost of care, and higher upside potential.
The transition to value-based care (VBC) has been tougher for traditional providers, which grapple with the challenges of heterogeneous patient and payer populations, along with financial, operational, and administrative hurdles. While some traditional providers have started to engage in VBC, true population-based reimbursement—such as partial- and full-capitation payment models and integrated payer-provider models—represents only around 7% of total healthcare spending today. But here, too, change is coming: According to Bain’s Front Line of Healthcare Survey, some 40% of primary care providers say the pandemic increased their interest in value-based payment models.
Looking ahead to 2030, we believe that a new breed of enablers—companies such as Agilon Health and Privia Health—will lead a movement of traditional independent providers to VBC. These companies will be agents of change, arming traditional providers with population health analytics, data integration, and care coordination tools, as well as the processes and people they need to succeed.
Care models in 2030
Increased cost awareness, consumerism, digital adoption, and physician shortages are putting pressure on today’s care models. In response, we expect a heightened focus on specific populations, broader adoption of multidisciplinary care teams, and growth of alternative sites and channels of care to redefine this space.
Population-specific scopes. Today, most physicians care for populations of patients with widely varying needs and diverse payers. But the recent success of APCs’ population-specific models has illuminated an alternative path forward for primary care providers.
Population-specific scopes in Medicare Advantage (MA) and Medicaid have several benefits, including a narrower payer environment and higher, risk-adjusted per-member-per-month rates. This allows providers to invest in resources and capabilities tailored to the patient population for more coordinated and comprehensive care delivery. While population-specific models currently account for less than 2% of the total market, we expect APCs will continue to innovate in MA and Medicaid, propelling growth in these segments.
There’s also room for experimentation in the commercial segment. Here, providers face distinct challenges, such as increased patient and payer diversity, as well as patient churn in employer segments. But compared with the traditional one-size-fits-all approach, APCs directed at narrower populations of self-funded employers may still offer a better opportunity to tailor capability investments to customer needs.
Higher cost pressures and physician shortages. As the industry wrestles with rising cost pressures and mounting labor shortages, leading primary care providers will get creative.
Most care is currently delivered through physician-centric teams: More than 70% of physicians don’t work alongside other specialists, and more than 45% don’t work alongside advanced practice providers (APPs). That won’t be sustainable by 2030.
We expect leading primary care providers to function in multidisciplinary care teams (MDCTs), with an integrated approach to medical, behavioral, and social determinants of health. In an environment where all team members are working at the top of their licenses, MDCTs can help optimize care delivery to advance patient outcomes. They can also promote health equity, which we expect to be a top priority for state governments, payers, and providers over the next decade.
But MDCTs won’t be enough to combat labor shortages. By 2030, the US will be short 45,000 primary care physicians. To effectively deliver care, organizations will have to rely more on APPs, especially in alternative sites and channels, such as retail health or virtual care. APPs will likely continue to focus on routine and urgent care while physicians quarterback care for the most complex cases, including patients with uncertain diagnoses. Projections show the APP labor force will grow sufficiently to meet this demand. In fact, some APC disrupters are already investing in this future talent pipeline. For instance, Oak Street Health is launching a new, graduate-level nurse practitioner training program.
Advances in technology can also alleviate industrywide pressures while dramatically improving the patient experience and clinical outcomes. For today’s patients, healthcare can be a painful piecemeal experience, from the struggle to find an available and affordable doctor to confusion over payments. By 2030, as more primary care providers transition into value-based care, technology adoption will accelerate—from the superficial, like electronic health record apps, to the truly transformative, like care management and workflow optimization platforms. Fast-growing APC models will lead the pack with seamlessly integrated experiences that benefit patients and clinicians alike.
Alternative sites and channels of care. Sites of care are moving from clinics to homes, retailers, and digital platforms. Retail giants like CVS, Walgreens, and Walmart have recently forayed into comprehensive primary care, with high ambitions for future expansion. And during the pandemic, 18% of primary care visits were virtual—soaring from a mere 1% in 2018.
These alternative sites and channels of care aren’t going anywhere. Although the share of virtual primary care settled around 12% at the end of 2021, it has earned patients’ and physicians’ trust, becoming a permanent fixture in the healthcare landscape. At the same time, patients still prefer to see their own doctor, and the need for physical examinations will always prevail. Given these considerations, we expect primary care providers with an omnichannel presence to excel over pure-play virtual providers.
That bodes well for many retailers, as they look to build comprehensive, omnichannel primary care. To grow their limited primary care clinics, retailers will likely partner with APC models and tap into APPs to build their labor force. Winners will also invest in care management and MDCTs to effectively serve patients with complex conditions across sites of care.
Ownership models in 2030
Finally, as reimbursement and care models shift, owners and investors will have to change their approach. More than half of primary care physicians are affiliated with a health system currently, compared with 38% of physicians in 2016. In 2030, we expect to see two major strategies for health systems and primary care. Some health systems will shift their strategic focus from acquisitions of primary care practices to partnerships. Recognizing that they can continue to spur referrals without primary care ownership by demonstrating quality and cost outcomes, these health systems will aim to become the preferred partner of APCs.
Other progressive health systems will transform their existing primary care practices into APCs, in an effort to deliver customer experiences and outcomes that will generate sustainable, profitable businesses. And more small practices will manage to stay independent, using enabler companies, like Agilon Health and Privia Health, to move into value-based care and become more profitable.
Meanwhile, payers will continue to grow their market share. Entering primary care in 2011, payers and payer-owned services companies already hold around 5% of the market, care for approximately 13 million lives, and employ around 12,000 physicians. That trajectory is set to continue. Payers will increasingly acquire well-coordinated, high-functioning practices, as well as the technological and digital capabilities required to scale risk-bearing models.
Private equity will also claim a larger share of the primary care space as investor interest holds steady. We anticipate increased consolidation of private equity– and venture capital–backed market disrupters throughout the next decade. Humana’s investment in CenterWell Senior Primary Care facilities as a joint venture with private equity firm Welsh, Carson, Anderson & Stowe is just one example of the growing trend of payer- and private equity–backed APCs.
A new competitive landscape
Amid this deluge of changes, how will the primary care landscape shake out? As reimbursement, care, and ownership models evolve, nontraditional providers will likely capture around 30% of the market (see Figure 1).
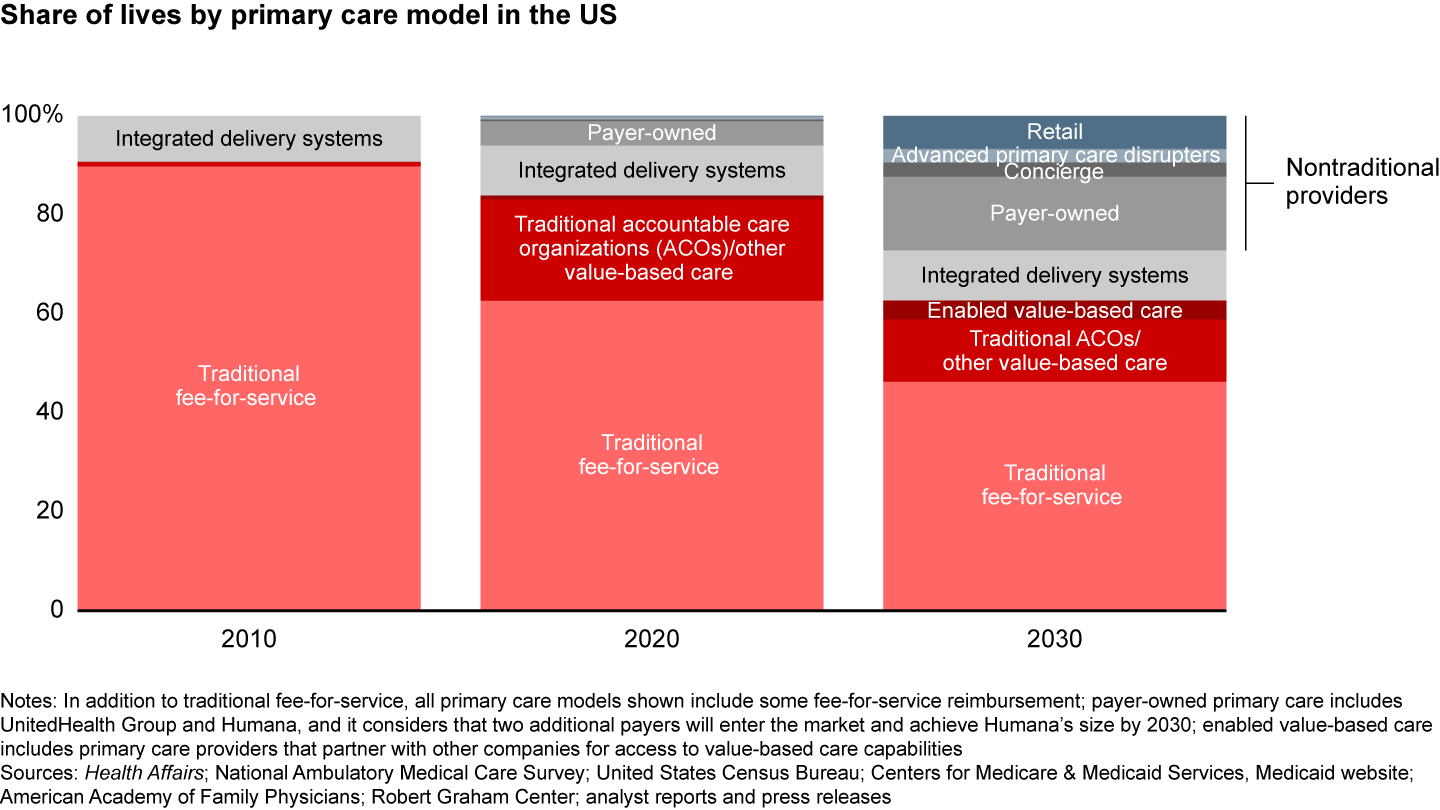

Five major competitive dynamics will define market share in this new era.
1. Risk-bearing, population-specific models will scale. Fully capitated APCs, led by disrupters and payers, will grow nationally. They will add value by mitigating administrative complexity for clinicians and improving patient outcomes through tailored offerings and enhanced care coordination. Many APCs demonstrate success in Medicare Advantage today, particularly due to favorable risk adjustment. But as risk adjustment factor methodology changes and APCs look to take on other populations, like commercial members, the winners of the future will be those that excel at improving clinical outcomes and reducing costs in order to be profitable.
2. Payers and payer-owned services companies will become one of the largest models. As they continue to pursue vertical integration strategies, UnitedHealth’s OptumCare and Humana, along with potential future market entrants, could serve around 15% of primary care lives by 2030.
3. Retailers will grab market share with full-scope primary care. Retail behemoths could account for 5% to 10% of total primary care lives by 2030. They will likely outperform traditional primary care providers on the patient experience, attracting customers through increased access and convenience, particularly in geographically underserved areas.
4. Alternative models will squeeze traditional models. Traditional fee-for-service providers will remain the largest primary care model in 2030, but they could lose around 15 to 20 percentage points of market share. Without infusions of capital to address administrative and operational obstacles, many of these providers will struggle to transition to fee-for-value. They will lag in improving outcomes and experiences for an increasingly aware and empowered patient population. They may also struggle to hire physicians. Traditional models will be competing with advanced models that have invested in developing a better physician experience, including improved clinical and administrative workflows, and collaborative team-based care that allows physicians to work at the top of their licenses.
5. Virtual channels will endure. Virtual care is set to grow across all primary care models, climbing back up to early-pandemic levels of approximately 20% penetration by 2030. That number could be even higher among young and healthy patients.
The road to 2030
The future state of primary care holds different implications for payers, health systems, and investors. Organizations will need to make complex strategic choices around where to play and how to win in this new landscape. Leadership teams can start by asking themselves a set of relevant questions.
Payers:
- As we make plays in primary care, which populations will we focus on? Will we invest in care delivery ownership or enablement? What are the strategic trade-offs of each?
- If we decide not to invest in ownership, how will we minimize the risk of being disintermediated by APCs and retailers—organizations that could contract directly with the government?
Health systems:
- In a world where new primary care models increasingly address consumer needs, improve quality, and reduce costs, how can we effectively protect our position in primary care?
- As we think about growth, can we partner with local APCs to boost referral volume without owning primary care practices? Or do we have the capabilities to develop or acquire APC models?
Investors:
- Which primary care models are most attractive—from enablers, to APCs, to high-functioning practices—when considering population focus and current valuations?
- Where could there be joint venture opportunities—for instance, with payers, retailers, or health systems—to support the growth of alternative primary care providers?